A Comprehensive Guide to the Contraceptive Pill Brands

Medically reviewed by
Dr Babak AshrafiLast reviewed: 18 Jul 2023
Contraceptive pills in the UK come under a variety of brand names from a number of different manufacturers. Most contraceptive pill brands are a unique combination of active ingredients and doses, but some are actually the same.
Figuring out what brands to choose can be confusing, so we’re going to try and shed some light on the differences between brands and what you need to know to make an informed choice about the right brand of pill for you.

What is meant by contraceptive pill brands?
A contraceptive pill brand refers to a contraceptive pill that is sold under a particular brand name. Different brands work slightly differently based on what hormones they have and how they’re taken. Different brands can have different manufacturers (companies responsible for making and selling them), but some manufacturers sell multiple brands of pill.
Unlike other medications that usually have branded and generic names, contraceptive pills are usually only sold under brand names. A generic is the non-branded name for a medication, which is normally the same as the active ingredient, like aspirin or paracetamol.
Part of the reason contraceptive pill names are usually branded is that there are a lot of different active ingredients and dosage combinations, especially with combined pills. Branded names are easier to recognise and search for, making it less complicated to find the right pill for you.
Branded medications are checked to the same safety standards as generic medications when licences are issued. In the UK, the Medicines and Healthcare products Regulatory Agency is in charge of regulating medications.
What different types of contraceptive pills are there?
There are a wide variety of contraceptive pill brands in the UK, but they can be sorted into a few different categories, which make them easier to compare. These include:
- combined and mini pills
- low-oestrogen combined pills
- monophasic and phasic combined pills
Popular contraceptive pills from our patients
How do different contraceptive pills work?
Most of the pills work in a similar way, with the main difference being whether they are combined or mini pills. Combined pills work by:
- preventing the ovaries from releasing any eggs
- making the mucus at the opening of the womb thicker
- the womb’s lining thinner, so fertilised eggs can’t attach themselves
Mini pills work in a similar way, but some of them don’t prevent eggs from being released.
Even though they work slightly differently, combined and mini pills are both over 99% effective when taken properly. Contraceptive pills also have a few advantages over other types of contraceptives, including:
- easy to stop and start
- no need to interrupt sex to use them
- can be delivered to your door with online doctor services like ZAVA
- no insertion or injection like coils or the hormonal injection
- some brands are available over-the-counter
-
-
The combined pill is called that because it contains a combination of two man-made hormones, progesterone and oestrogen. This means it has some benefits over the mini pill, which only contains progesterone, including:
- stopping ovulation
- less chance of progesterone-only side effects, like mood swings or acne
- improvements to some health conditions, including: premenstrual syndrome or premenstrual dysphoric disorder, polycystic ovary syndrome, acne, perimenopause
Advantages and disadvantages of the combined pill
Combined pill pros compared to the mini pill:
- Bigger ‘window of opportunity’ to take your pill – 24 hours, instead of 12 or 3 hours for the mini pill
- Extra benefits from oestrogen, like helping acne or premenstrual syndrome
- Less progesterone-only side effects, like mood swings and acne
Combined pill cons compared to the mini pill:
- Not suitable for some people (see below)
- A higher risk of oestrogen-related side effects, like breast tenderness, nausea and headaches
- Not available over-the-counter, when some mini pills are
People who can’t use the combined pill include:
- people who are breastfeeding less than 6 weeks after childbirth
- smokers over 35
- people with high blood pressure
- people with a history of blood clots
- people who get migraines with auras
- people who have a history of heart disease
- people who have a BMI over 35
Combined contraceptive pill side effects
Possible side effects of the combined pill include:
- breakthrough bleeding or spotting
- breast tenderness
- headaches
- nausea (feeling sick)
- feeling bloated
- high blood pressure
-
-
Unlike the combined pill, the mini pill only contains one man-made hormone, progesterone. This means it has some benefits over the combined pill because it doesn’t have oestrogen in it, including:
- some brands available over-the-counter
- no oestrogen-related side effects like nausea or breast tenderness
- extra improvements to some health conditions, including: endometriosis, heavy periods
It’s safe for some women where the combined pill isn’t, such as people:
- aged over 35 who smoke
- who are overweight
- who are breastfeeding less than 6 weeks after childbirth
- who get migraines with auras
- with a history of heart disease
- with high blood pressure
- with a higher risk of blood clots
Not all mini pills work the same way. Some stop working if you forget a dose for more than 3 hours, but some can be left as late as 12 hours before you’re at risk of pregnancy.
Advantages and disadvantages of the mini pill
Advantages of the mini pill over the combined pill include:
- being safe for women with certain conditions
- less chance of oestrogen-related side effects, like breast tenderness, headaches or nausea
- some brands are available over-the-counter
- extra benefits to endometriosis and periods
Disadvantages compared to the combined pill include:
- shorter window of opportunity for taking them
- higher chance of progesterone-only side effects, like mood swings and acne
- no oestrogen-related benefits, like improving acne or premenstrual syndrome
Mini pill side effects
Possible mini pill side effects include:
- acne
- breast tenderness
- low sex drive
- mood changes
- headaches
- nausea (feeling sick)
- ovarian cysts
-
-
Low-dose combined pills have less oestrogen in them, but they’re still just as effective. Because they have a lower dose of oestrogen, it means the effects or chances of some of the benefits and side effects are different compared to high-oestrogen pills.
Combined pills can have anywhere from 20 to 50 micrograms of oestrogen in them. A low-dose pill is considered to be any pill that has 30 micrograms or less.
Some of the benefits increased by low-oestrogen pills are:
- less chance of oestrogen-related side effects, like breast tenderness, headaches and nausea
- improvements to polycystic ovary syndrome, especially if the progesterone in the pill has less androgenic (male hormone) effect
Low-dose pill side effects
Side effects of the low oestrogens pills are the same as normal combined pills, it’s just that a few of them are less likely. Side effects of low-dose pills still include:
- breakthrough bleeding or spotting
- breast tenderness
- headaches
- nausea (feeling sick)
- feeling bloated
- high blood pressure
-
-
Monophasic pill brands are actually the majority of combined pill brands. All monophasic pills contain just one dose of their active ingredients, which are taken through the course of treatment.
This is compared to phasic pills, which have different doses of active ingredients that you take during a 28-day cycle. Phasic pills have different doses because they are supposed to copy your natural hormone cycle that you’d experience during a 28-day period cycle. But, research shows this doesn’t have any proven benefits over monophasic pills.
What are monophasic 21-day pills?
Again, monophasic 21-day pills are the most common kinds of combined pills. These are meant to be taken for 21 days straight, and then you can take a seven-day break. Although you don’t actually need to take the break if you don’t want to, manufacturers usually licence combined pills to be taken with a break.
Compared to 21-day pills, every-day pills include 7 hormone-free pills you take during your break. This is to make it easier to keep track of your doses and doesn’t affect how they work.
Monophasic pill side effects
Monophasic pills have exactly the same side effects as phasic pills. There’s no difference in your chance of getting side effects, either. Possible side effects include:
- breakthrough bleeding or spotting
- breast tenderness
- headaches
- nausea (feeling sick)
- feeling bloated
- high blood pressure
What is the best combined pill brand?
All brands of combined pills are just as effective when taken properly. But, they do contain different ingredients and doses, which different people can react differently to.
Below are some popular UK brands of combined contraceptive pills for you to consider.
Rigevidon pill
- Contains 150 micrograms of levonorgestrel and 30 micrograms of ethinylestradiol
- Is a second-generation pill
- Similar pills include: Levest, Ovranette
Levonorgestrel and ethinylestradiol pills like the Rigevidon pill were introduced in the 70s. It’s considered a second-generation pill because the progesterone levonorgestrel was discovered after the progesterones used in first generation pills and largely replaced them as a safer alternative. Unlike first generation pills, second-generation pills like Rigevidon are still widely used.
Microgynon 30
- Contains 150 micrograms of levonorgestrel and 30 micrograms of ethinylestradiol
- A second-generation pill
- Similar pills include: Levest, Ovranette, Rigevidon
Microgynon 30 is a very similar pill to the one discussed above, Rigevidon. They both contain the same active ingredients in the same doses. Like the Rigevidon pill, Microgynon is a second generation pill containing levonorgestrel and is still widely used today.
Yasmin Pill
- Contains 3 milligrams drospirenone and 30 micrograms ethinylestradiol
- A fourth-generation pill
- Similar pills include: Eloine, Lucette
The progesterone in Yasmin, drospirenone, was patented in 1976 but not used medically until 2000. Called a fourth-generation progesterone, it has less of an androgenic (male hormone) effect, making it less likely to cause acne but also less effective for treating endometriosis. On the other hand, drospirenone comes with a slightly higher risk of blood clots, although it’s still very low. Overall, drospirenone combined pills are generally safe and suit many women better in terms of side effects.
Marvelon pill
- Contains 150 micrograms of desogestrel and 30 micrograms of ethinylestradiol
- A third-generation pill
- Similar pills include: Gedarel, Lucette, Mercilon
Marvelon contains the third-generation progesterone desogestrel, which was discovered in 1972 and became available for use in Europe in 1981. This progesterone causes less androgenic and estrogenic activity (involving male and female hormones), which means the side effects and benefits of both of these hormones may be reduced. But, like drospirenone pills, desogestrel pills come with a slightly higher risk of blood clots, although they’re safe and well-tolerated overall.
Lucette pill
- Contains 3 milligrams drospirenone and 30 micrograms ethinylestradiol
- A fourth-generation pill
- Similar pills include: Eloine, Yasmin
Very similar to Yasmin pill, Lucette contains the same hormones in the same doses, including the fourth-generation progesterone drospirenone. This means it also has less androgenic (male hormone) effect and has a lower risk of some side effects, but like Yasmin, the drospirenone comes with a slightly higher risk of blood clots. Still, Lucette is safe if approved by a doctor.
According to a study by University College London of contraceptive pill prescribing trends between 2000 and 2018, the percentage of people being prescribed the combined pill dropped from 26% to 14% during the 18-year period. They also found that the percentage of people being prescribed the mini pill went up from 4% to 11% during the same period.
What are the best mini pill brands?
Like combined pills, there’s no single mini pill brand that is right for everyone. Finding one that works for you can take some trial and error. Mini pills with a 12-hour window can be good for people who forget to take their pill on time.
Even so, all mini pills can be equally as effective. Below we go into detail on some of the more popular brands.
Cerelle pill
- Contains 75 micrograms of desogestrel
- A 12-hour window mini pill
- Contains a third-generation progesterone
- Similar pills: Cerazette, Hana, Zelleta
The desogestrel in Cerelle is a third-generation progesterone, which was discovered in 1972. Because it has less androgenic (male hormone) effect, it causes less oily skin and can be less likely to cause acne than some other mini pills. It also has a 12-hour window compared to some other mini pills with only 3-hour windows. This means you can be up to 12 hours late taking it and it will still work.
Cerazette pill
- Contains 75 micrograms of desogestrel
- Is a 12-hour window mini pill
- Contains a third-generation progesterone
- Manufactured by Organon
- Similar pills: Cerelle, Hana, Zelleta
Cerazette contains the same active ingredient in the same dose as Cerelle. It works the same way, having less chance of causing acne and a 12-hour window for taking it.
Norgeston pill
- Contains 30 micrograms of levonorgestrel
- Is a 3-hour window mini pill
- Contains a second-generation progesterone
- No other pills have the same ingredients
Compared to third-generation progesterones, the levonorgestrel in Norgeston has an increased androgenic (male hormone) effect. This means it can make acne more likely, but it can also have a bigger positive effect on endometriosis and heavy periods.
Hana pill
- Contains 75 micrograms of desogestrel
- Is a 12-hour window mini pill
- Contains a third-generation progesterone
- Similar pills include: Cerazette, Cerelle
Just like Cerelle and Cerazette, Hana also contains desogestrel at the same dose. So it’s got the same reduced chance of acne and a 12-hour window for taking it.
Noriday pill
- Contains 350 micrograms of norethisterone
- Is a 3-hour window mini pill
- Contains a first-generation progesterone
- No other pills have the same ingredients
Noriday contains a first generation progesterone. While these aren’t widely used in combined pills any more, it works fine as a mini pill progesterone. It has less androgenic effect than second-generation progesterones, but more than third-generation ones. This means it falls somewhere in the middle on acne, endometriosis and heavy periods.
So which contraceptive pill brand is best for me?
Which pill is best for you will depend on:
- your current and past health conditions
- what side effects you’re looking to avoid
- what benefits you want from your pill
- if you’re likely to forget doses
If you’re still not sure which pill to choose, a healthcare professional can give you advice. ZAVA’s online doctor service can review your situation through our assessment and check whether the pill you request is right for you and suggest alternatives if it isn’t.
Frequently asked questions
Where can I get the contraceptive pill?
You can get the contraceptive pill over-the-counter for certain brands of mini pill, from a nurse or doctor at your GP surgery or a sexual health clinic or online from an online doctor service like ZAVA.
ZAVA lets you request treatment online without a face-to-face appointment through a simple online assessment, and if your request is approved, it’s delivered right to your door.
What is the most common birth control pill brand?
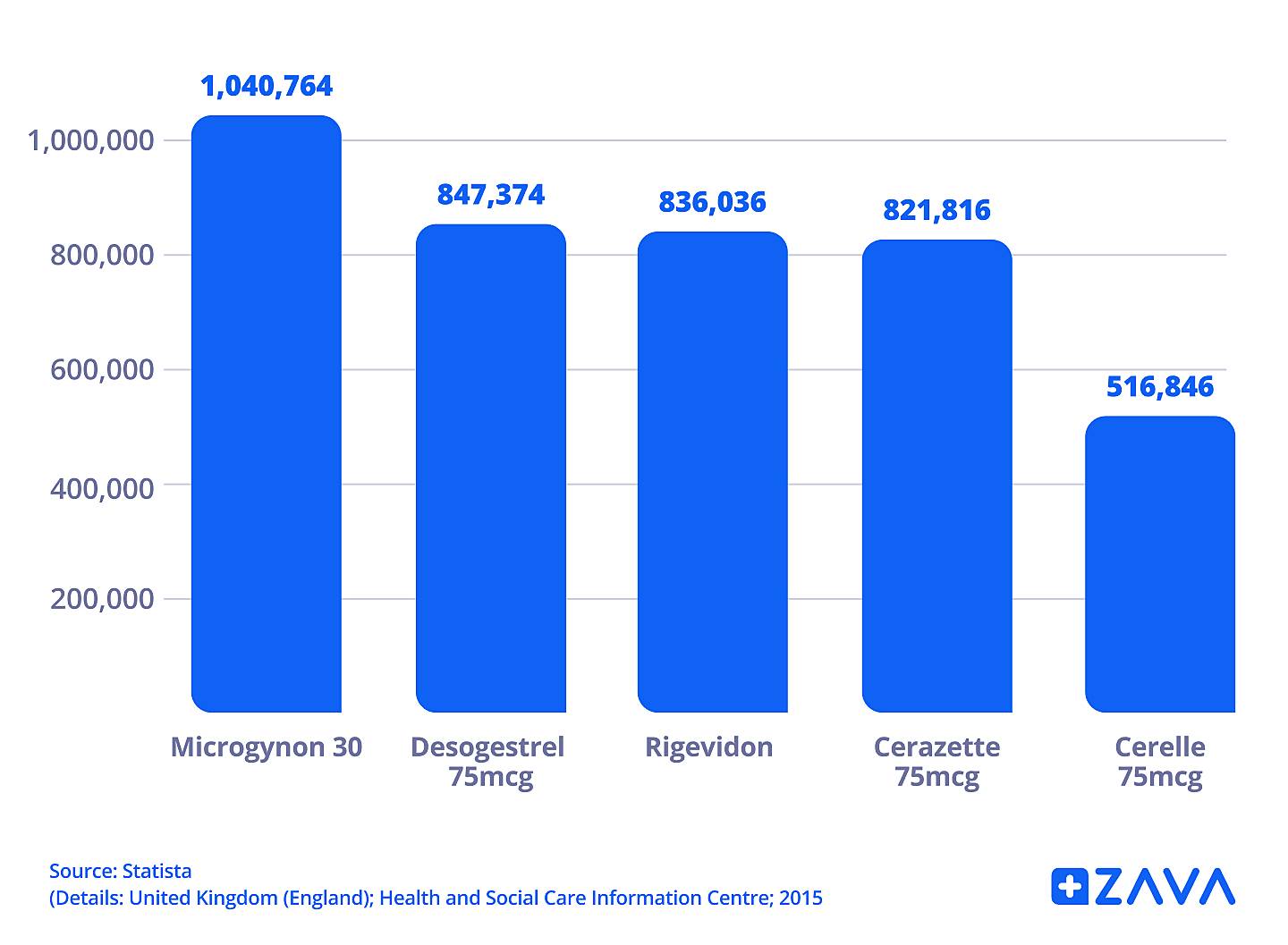
Pills can go in and out of fashion as people learn about and try different brands. Microgynon is generally the most widely used in the UK.
What is the best contraceptive pill for anxiety and depression?
There’s no one best pill brand for anxiety and depression. All brands of combined pills will be better at avoiding these side effects than mini pills. This is because these side effects tend to be worse when progesterone is used alone. The oestrogen in combined pills helps reduce this effect.
Can I take a different brand of birth control?
If you’re already on a brand of birth control, then switching is possible. A doctor can help you switch from one brand to another, even between combined pills and mini pills. You can also tell our doctors what pill you’re on during a ZAVA assessment and then can help you switch.
Is Rigevidon a monophasic pill?
Yes, Rigevidon is a monophasic pill. This means it only uses one dose of ingredients throughout the whole course of treatment. In this case, Rigevidon contains 150 micrograms of levonorgestrel and 30 micrograms of ethinylestradiol and these doses don’t change.
What are the top 5 contraceptives?
Different contraceptives suit different people so it’s hard to say what ‘top’ contraceptives will be for you. Many contraceptives are over 99% effective when used properly, although some can be less effective because people don’t always use them properly, like the pill.
Below are a list of the most effective contraceptives when you take into account people using some wrongly:
- Male sterilisation, permanent but effective if the procedure is successful.
- Female sterilisation, just like male sterilisation it’s very effective but permanent.
- Intrauterine device, often called ‘the coil’ this contraceptive is very effective when inserted correctly.
- Intrauterine system, similar to the coil and just as effective.
- Contraceptive implant, inserted under the skin and effective and reliable.

Dr Babak Ashrafi Clinical Lead for Service Expansion
Accreditations: BSc, MBBS, MRCGP (2008)
Babak studied medicine at King’s College London and graduated in 2003, having also gained a bachelor’s degree in Physiology during his time there. He completed his general practice (GP) training in East London, where he worked for a number of years as a partner at a large inner-city GP practice. He completed the Royal College of GPs membership exam in 2007.
Meet our doctorsLast reviewed: 18 Jul 2023
-
https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD003553.pub3/full [accessed 26/06/23]
-
https://www.nhs.uk/conditions/contraception/the-pill-progestogen-only/ [accessed 26/06/23]
-
Combined pill - NHS (www.nhs.uk) [accessed 26/06/23]